The birth of Hugo Powell marks a historic milestone in British medical history, representing the first time a baby has been born in the United Kingdom to a mother who received a womb transplant from a deceased donor. Delivered at Queen Charlotte’s and Chelsea Hospital in London, Hugo entered the world weighing 3.09 kilograms (6lb 13oz), bringing immeasurable joy to his mother, Grace Bell, and her partner, Steve Powell.
For Bell, who was born without a functioning womb due to a rare congenital condition, the arrival of her son is nothing short of life-changing. Her journey reflects not only the rapid advancement of transplant medicine but also the profound generosity of organ donation and the dedication of specialist surgical teams who have worked for years to make such outcomes possible.
Hugo’s birth places the United Kingdom among a small number of countries to achieve a successful live birth following a deceased donor womb transplant. While womb transplantation has been developing internationally for over a decade, this case stands out as the first of its kind in Britain using an organ from a donor who had died. The achievement underscores the growing possibilities in reproductive medicine and offers renewed hope to women affected by uterine factor infertility.
A Medical Breakthrough Years in the Making
Grace Bell was born with Mayer-Rokitansky-Küster-Hauser syndrome, commonly known as MRKH, a rare condition that results in an underdeveloped or absent uterus while leaving the ovaries intact. Women with MRKH typically learn in adolescence that they are unable to carry a pregnancy. For Bell, that diagnosis meant being told as a teenager that she would never be able to experience pregnancy. Like many women with the condition, she faced the prospect of parenthood through alternatives such as adoption or surrogacy.
The possibility of womb transplantation has gradually transformed that landscape. In 2024, Bell underwent a groundbreaking transplant procedure in which she received a uterus from a deceased donor. The surgery was conducted by a specialist team associated with Womb Transplant UK, led clinically by Professor Richard Smith, a consultant gynaecological surgeon at Imperial College Healthcare NHS Trust. The procedure required meticulous coordination, including organ retrieval, vascular connection, and careful postoperative monitoring to ensure that the transplanted organ functioned properly.
Several months after recovering from the transplant, Bell began fertility treatment. Because women undergoing womb transplantation typically use embryos created via in vitro fertilisation prior to the transplant, the process involves careful planning. The transplanted uterus must establish sufficient blood supply and demonstrate normal function before embryo transfer can take place. In Bell’s case, the process was successful, and she became pregnant later that year. Hugo was born in December, marking the culmination of years of research, surgical refinement, and personal resilience.
UK welcomes first baby after womb transplant from dead donor
— WuzupNigeria (@WuzupNigeria) February 24, 2026
A baby boy named Hugo Richard Norman Powell has made medical history in the United Kingdom as the first child born to a mother who received a womb transplant from a deceased donor.
Hugo was delivered in December pic.twitter.com/eXuDvZpbZQ
Globally, approximately 25 to 30 babies have been born following deceased donor womb transplants, with most womb transplants worldwide involving living donors. The UK had previously carried out a womb transplant in 2023 involving a living donor, when another MRKH patient received a uterus from her sister. However, Hugo’s birth represents the first time in the country that a womb from a deceased donor has resulted in a live birth. Across Europe, only two similar cases had been reported before this one, highlighting the rarity and significance of the achievement.
The Human Story Behind the Science
While the medical aspects of Hugo Powell’s birth are remarkable, the human dimensions are equally powerful. Bell has described her son’s arrival as a “miracle,” expressing that she never believed such an outcome would be possible in her lifetime. Her words reflect the emotional impact of the journey, which began with a devastating diagnosis in adolescence and culminated in motherhood years later.
Central to this story is the anonymous donor and her family. The womb transplanted into Bell came from a woman who had died, and five other organs from the same donor were transplanted into four additional recipients, saving or transforming multiple lives. Organ donation in this case extended beyond life-saving interventions to enabling life itself. Bell has spoken of thinking about her donor every day and feeling immense gratitude toward the donor’s family for their generosity during a time of profound grief.
Read : 21-Year-Old BYU Wide Receiver Parker Kingston Charged with First-Degree Felony Rape
The donor’s parents have also shared their perspective, describing the shattering loss of their daughter while expressing pride in the legacy she has left. Through organ donation, they emphasised, their daughter provided other families with time, healing, hope, and now the gift of new life. Their decision underscores the deeply personal nature of organ donation and its capacity to create enduring impact even after tragedy.
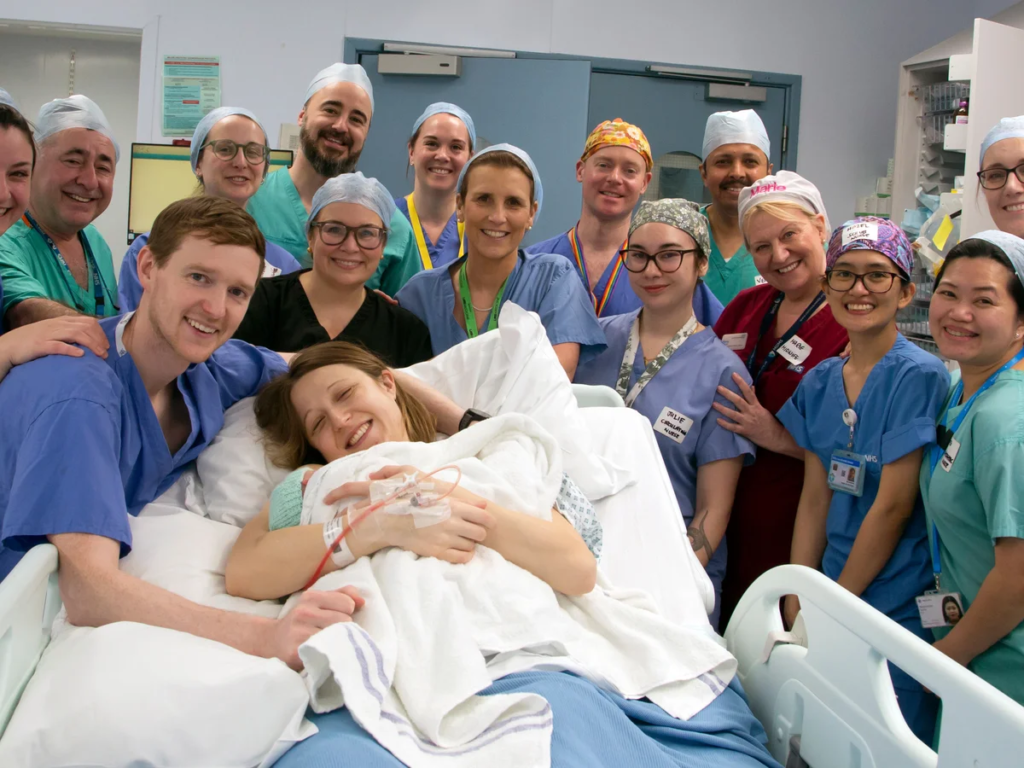
The naming of Hugo’s middle name, Richard, after Professor Smith, further highlights the close bond formed between the family and the medical team. Smith, who was present at the birth, described the journey as extraordinary and acknowledged the years of commitment from the multidisciplinary team that made the outcome possible. Surgeons, fertility specialists, transplant coordinators, nurses, and researchers all contributed to the complex pathway from transplantation to childbirth.
Beyond the immediate family and clinical team, Hugo’s birth resonates with women across the UK and internationally who live with uterine factor infertility. For many, the case offers tangible evidence that carrying a pregnancy may become a realistic possibility. Although womb transplantation remains a highly specialised and resource-intensive procedure, each successful birth strengthens the clinical knowledge base and informs future practice.
Ethics, Consent, and the Future of Womb Donation
Womb transplantation presents unique ethical and logistical considerations compared with other forms of organ donation. Unlike kidneys, livers, or hearts, the uterus is not a life-saving organ but a life-enabling one. As a result, it is not covered under standard organ donor registration or deemed consent systems in the UK. Families must be asked specifically whether they are willing to donate a womb, making informed discussions and clear consent processes essential.
The procedure also involves long-term considerations for recipients. Women who receive a transplanted womb must take immunosuppressant drugs to prevent rejection of the organ. These medications carry risks if taken indefinitely. For this reason, the transplanted uterus is typically removed once the recipient has completed her family, allowing her to discontinue immunosuppressive therapy. Bell and her partner have indicated that the organ will be removed after they have finished having children, reflecting the temporary nature of the transplant.

As more cases are undertaken worldwide, data continues to accumulate regarding safety, outcomes, and long-term implications. More than two-thirds of womb transplants globally have involved living donors, often close relatives such as mothers or sisters. Living donation eliminates some uncertainties associated with deceased donor retrieval but raises its own ethical questions, including surgical risk to the donor.
Deceased donor transplantation, while technically demanding due to time constraints and organ preservation challenges, avoids exposing a living person to major surgery for a non-life-saving purpose. The success of Hugo’s birth may encourage broader public awareness about womb donation and stimulate discussion about whether consent systems should evolve to include the uterus more routinely. However, such changes would require careful ethical review and public engagement. Medical teams must also consider equitable access, funding models, and the psychological support required for recipients and donors’ families alike.
From a clinical perspective, continued research will focus on refining surgical techniques, reducing rejection rates, and improving pregnancy outcomes. Each successful birth contributes valuable insight into vascular connections, immunosuppressive protocols, and obstetric management in transplanted uteri. As expertise grows, the procedure may become more widely available, though it is likely to remain specialised for the foreseeable future.
For Grace Bell and Steve Powell, the broader policy discussions are secondary to the reality of their son’s arrival. After years of uncertainty, they have welcomed Hugo into their lives, marking a moment that blends scientific progress with deeply personal fulfilment. Hugo’s birth stands as a testament to medical innovation, the courage of patients willing to undergo pioneering treatment, and the compassion of a donor family whose decision made this milestone possible.

